Greenish blood may be caused by rare conditions like sulfhemoglobinemia, affecting hemoglobin and oxygen transport. It can indicate serious underlying issues, requiring medical attention. Understanding symptoms and causes helps in early diagnosis and timely treatment.
The Science Behind Blood Color
The vibrant red color of human blood is entirely dependent on a protein called hemoglobin, which is packed inside our red blood cells. Hemoglobin is responsible for grabbing oxygen from the lungs and delivering it to tissues throughout the body. This process is essential for survival, as every organ depends on a constant oxygen supply to function properly.
The key to this oxygen-carrying capability—and the red color of blood—is iron. Each hemoglobin molecule contains iron-rich heme groups. When oxygen binds to these iron atoms, the interaction causes the blood to reflect bright red light. Oxygen-rich blood flowing through the arteries appears bright cherry red, while oxygen-depleted blood returning through the veins appears darker red.
Without this iron-oxygen bond, normal blood color and oxygen transport would not be possible. This is why any disruption in hemoglobin structure or iron chemistry can affect blood appearance and function.
When Blood Color Changes (Greenish Blood and Other Rare Cases)
 In rare medical conditions, blood color can change due to chemical alterations in hemoglobin. One such condition is sulfhemoglobinemia, which is linked to unusual cases of greenish blood.
In rare medical conditions, blood color can change due to chemical alterations in hemoglobin. One such condition is sulfhemoglobinemia, which is linked to unusual cases of greenish blood.
In these rare situations, sulfur becomes incorporated into hemoglobin molecules, preventing normal oxygen binding. As a result, the blood may appear greenish or dark abnormal in color instead of red.
Understanding greenish blood causes is important because it may indicate underlying exposure to certain medications, chemicals, or metabolic disorders. Although rare, such blood color changes require medical evaluation.
Role of Hemoglobin in Blood Color and Health
Hemoglobin is not only responsible for blood color but also plays a vital role in maintaining oxygen balance throughout the body. It ensures that oxygen from the lungs is transported to tissues and organs, supporting essential life functions.
Any disruption in hemoglobin structure or function can lead to noticeable symptoms such as fatigue, shortness of breath, dizziness, and abnormal blood appearance. In severe cases, oxygen delivery becomes inefficient, affecting organ performance and overall health.
Conditions affecting hemoglobin, including methemoglobinemia and sulfhemoglobinemia, highlight how sensitive blood chemistry truly is. These disorders can lead to unusual blood color changes, which may sometimes be confused with other serious medical conditions. Proper diagnosis is essential to identify the exact cause.
Why Iron is Essential for Normal Blood Color
Iron is a key component of hemoglobin and plays a central role in maintaining healthy blood function. It allows hemoglobin to bind with oxygen efficiently and gives blood its normal bright red color.
When iron levels are low, the body develops anemia, a condition where blood cannot carry enough oxygen. This often leads to symptoms like fatigue, weakness, pale skin, and reduced physical performance.
On the other hand, chemical disruptions involving iron or sulfur can result in rare blood disorders. These may include abnormal blood color changes such as greenish blood, bluish tones, or darkened blood appearance. Such changes indicate that the normal oxygen-transport system has been affected.
Maintaining proper iron balance through diet and medical care is therefore essential for healthy blood production and function.
Medical Importance of Blood Color Changes
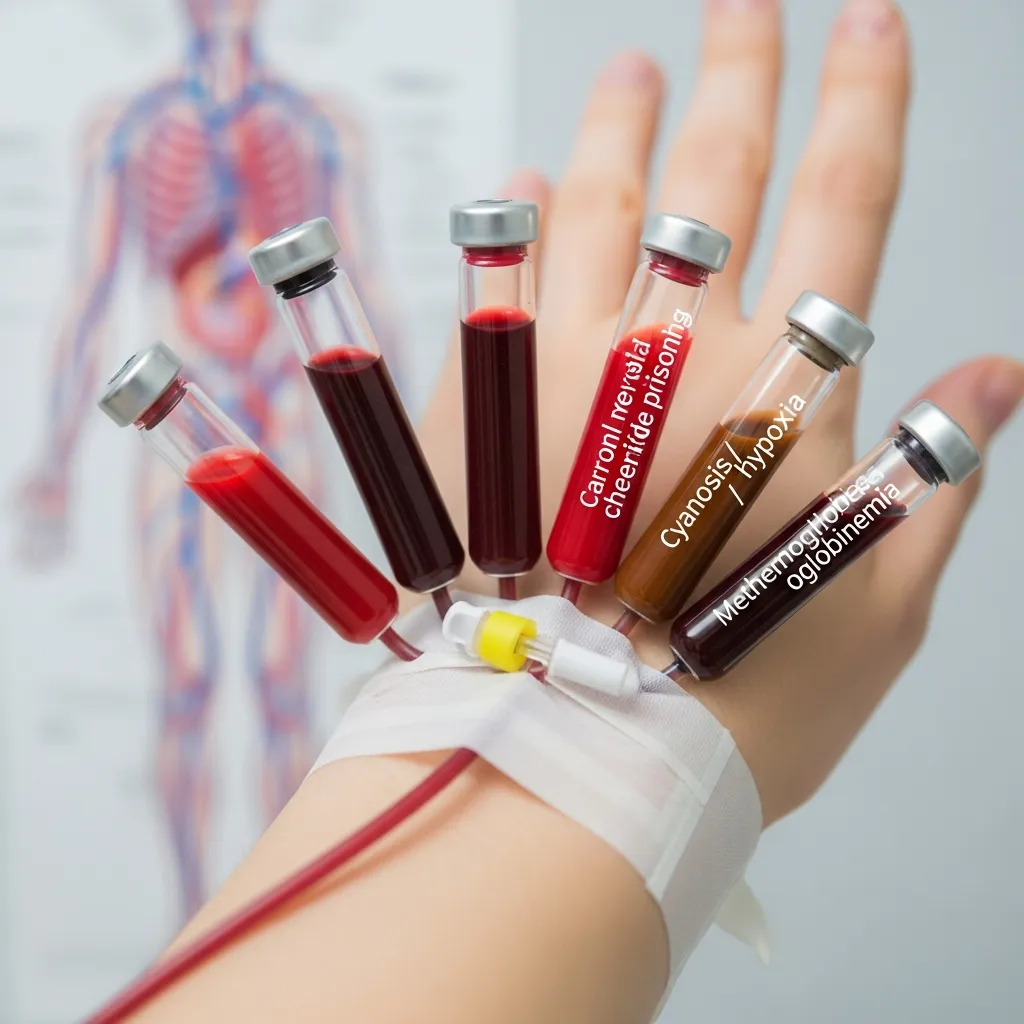 Changes in blood color, including rare cases of greenish blood, should always be taken seriously. While some discolorations may be temporary or harmless, others can indicate underlying metabolic or toxic conditions.
Changes in blood color, including rare cases of greenish blood, should always be taken seriously. While some discolorations may be temporary or harmless, others can indicate underlying metabolic or toxic conditions.
Doctors use a combination of diagnostic tools to evaluate abnormal blood color, including blood tests, oxygen saturation measurements, and specialized hemoglobin analysis. These tests help determine whether the issue is related to iron imbalance, oxygen deficiency, or chemical changes in hemoglobin.
Early diagnosis is extremely important because it allows timely treatment and helps prevent complications such as organ damage or prolonged oxygen deprivation.
When to Seek Medical Attention
Any persistent symptoms associated with abnormal blood function—such as unexplained fatigue, breathing difficulty, or visible changes in blood color—should be evaluated by a healthcare professional.
Even though rare conditions like greenish blood are uncommon, they may signal serious underlying issues that require prompt medical care. Early consultation ensures accurate diagnosis and improves treatment outcomes.
Causes of Greenish Blood
When blood appears green, it indicates a significant alteration in the hemoglobin molecule. The most common cause of greenish blood is a rare condition known as sulfhemoglobinemia.
Sulfhemoglobinemia
Sulfhemoglobinemia occurs when a sulfur atom incorporates itself into the hemoglobin molecule, creating a substance called sulfhemoglobin. Unlike normal hemoglobin, sulfhemoglobin cannot carry oxygen effectively. More visibly, the presence of the sulfur atom changes the way the molecule absorbs and reflects light, giving the blood a distinct greenish-black or dark green appearance.
The formation of sulfhemoglobin is usually triggered by exposure to certain sulfur-containing medications or chemicals. Common culprits include:
- Medications: High doses of certain drugs, particularly sulfonamide antibiotics, sumatriptan, and some migraine medications, can induce this condition. Overuse of phenazopyridine (often used for urinary tract pain) has also been linked to greenish blood.
- Environmental Exposure: Inhalation or occupational exposure to hydrogen sulfide gas can lead to the formation of sulfhemoglobin.
Diagnosis typically involves specialized blood tests, as standard pulse oximeters often misread oxygen levels in the presence of sulfhemoglobin.
Other Medical Conditions
While sulfhemoglobinemia is the primary cause of truly greenish blood, other severe medical conditions can cause blood to look unusually dark or discolored, sometimes appearing greenish under certain lighting:
- Severe Sepsis or Infection: Extreme systemic infections can sometimes alter blood chemistry and appearance, though rarely turning it overtly green.
- Poisoning: Ingestion of specific toxic chemicals can alter hemoglobin function and color.
- Rare Genetic Conditions: While genetic blood disorders, such as the alpha thalassemia trait, primarily affect the size and shape of red blood cells leading to anemia, they do not typically cause blood to turn green. However, understanding genetic variations in hemoglobin is crucial for overall blood health awareness.
Dietary Factors
It is a common myth that eating massive amounts of green vegetables can turn your blood green. While chlorophyll gives plants their green color and is structurally similar to heme, the human digestive system breaks it down completely. Dietary chlorophyll has no impact on the systemic color of human blood.
Distinguishing Greenish Blood from Other Abnormal Colors
Greenish blood is not the only type of abnormal blood color recognized in medical science. Changes in blood color are rare but important clinical signs that may indicate underlying chemical, oxygenation, or hemoglobin-related disorders. To understand greenish blood properly, it must be carefully distinguished from other abnormal blood color conditions such as bluish or brownish blood.
Accurate identification of blood discoloration is essential because different causes require different treatments. Laboratory testing, oxygen measurement, and hemoglobin analysis are usually needed to confirm the exact condition.
Bluish or Dark Blood (Methemoglobinemia)
Methemoglobinemia is a condition where the iron in hemoglobin is chemically altered from its normal state. In this form, hemoglobin is unable to bind and carry oxygen effectively, leading to reduced oxygen delivery throughout the body.
As a result, the blood may appear dark brown, bluish, or even chocolate-colored. Patients often show signs of cyanosis, where the skin, lips, or nails develop a bluish tint due to low oxygen levels.
Unlike greenish blood caused by sulfhemoglobinemia, methemoglobinemia is often reversible. In many cases, it can be treated quickly using a medication called methylene blue, which helps restore normal hemoglobin function and oxygen transport.
Brownish Blood and Oxygen Deprivation
 Brownish blood can also be a sign of methemoglobinemia or severe oxygen deficiency in the body. When blood is not properly oxygenated, it may lose its bright red appearance and turn darker or brownish in color.
Brownish blood can also be a sign of methemoglobinemia or severe oxygen deficiency in the body. When blood is not properly oxygenated, it may lose its bright red appearance and turn darker or brownish in color.
In some cases, severe dehydration or circulatory issues can also contribute to darker blood appearance due to reduced plasma volume and altered blood flow.
Although brownish blood may look similar to other abnormal conditions, it is clinically important because it often indicates poor oxygen delivery to tissues, which can become life-threatening if not treated.
Key Differences Between Greenish, Bluish, and Brownish Blood
Each abnormal blood color is linked to a different underlying mechanism:
- Greenish blood is most commonly associated with sulfhemoglobinemia, where sulfur compounds interfere with hemoglobin structure.
- Bluish or dark blood is often linked to methemoglobinemia, where oxygen binding is impaired.
- Brownish blood usually reflects severe oxygen deficiency or oxidized hemoglobin states.
Because these conditions can look similar externally, laboratory testing is essential for accurate diagnosis.
Why Accurate Diagnosis is Important
Misidentifying abnormal blood color conditions can delay proper treatment. For example, methemoglobinemia requires specific antidotal therapy, while sulfhemoglobinemia is managed differently and may take longer to resolve.
Doctors rely on blood gas analysis, co-oximetry, and detailed patient history to determine the exact cause of discoloration. Early detection improves outcomes and prevents complications related to oxygen deprivation.
Symptoms Associated with Greenish Blood
The symptoms of sulfhemoglobinemia and greenish blood are primarily related to the body’s sudden inability to transport oxygen effectively. Because sulfhemoglobin cannot carry oxygen, the body enters a state of hypoxia.
Common symptoms include:
- Cyanosis: A bluish or greenish tint to the skin, lips, and nail beds due to lack of oxygen.
- Fatigue and Weakness: A profound lack of energy as tissues are starved of oxygen.
- Shortness of Breath: Difficulty breathing as the body attempts to compensate for poor oxygen delivery.
- Dizziness and Confusion: Neurological symptoms resulting from inadequate oxygen reaching the brain.
- Organ Damage: In severe, untreated cases, prolonged oxygen deprivation can lead to damage to the heart, brain, and other vital organs.
Diagnosis and Treatment
Discovering greenish blood is a medical emergency that requires prompt diagnosis and intervention.
Diagnostic Steps
- Medical History: Doctors will urgently review any recent medications, dietary supplements, or potential chemical exposures to identify the trigger.
- Physical Examination: Assessing the extent of cyanosis and respiratory distress.
- Co-oximetry: Standard pulse oximeters are unreliable in these cases. Co-oximetry is a specialized blood test that can accurately measure the exact levels of normal hemoglobin, sulfhemoglobin, and methemoglobin in the blood.
Treatment Approaches
The primary treatment for greenish blood caused by sulfhemoglobinemia is supportive care and elimination of the offending agent.
- Removing the Cause: The most critical step is immediately stopping the medication or removing the patient from the chemical exposure that caused the condition.
- Supportive Care: Administering supplemental oxygen and providing intravenous fluids to support organ function.
- Blood Transfusion: Unlike methemoglobinemia, there is no specific antidote (like methylene blue) for sulfhemoglobinemia. The altered red blood cells must naturally reach the end of their lifespan (about 120 days). In severe cases where oxygen levels are critically low, an exchange blood transfusion may be necessary to rapidly replace the defective cells with healthy red blood cells.
Managing blood health also requires a broad understanding of other hemoglobin-related conditions, such as recognizing chipmunk facies thalassemia as a complication of severe bone marrow expansion in certain genetic disorders.
When to Seek Medical Attention
Abnormal blood color, or the sudden appearance of a bluish or greenish tint to your skin and lips, is a critical warning sign. This is not a condition that can be managed at home. If you or someone else experiences sudden shortness of breath, confusion, and visible cyanosis—especially after starting a new medication—seek emergency medical care immediately.
Prevention
 Preventing the rare occurrence of greenish blood primarily revolves around medication safety and occupational health.
Preventing the rare occurrence of greenish blood primarily revolves around medication safety and occupational health.
- Careful Medication Management: Always take prescription medications exactly as directed. Never exceed the recommended dose of over-the-counter pain relievers like phenazopyridine. Ensure your healthcare provider is aware of all the medications and supplements you are taking to prevent dangerous drug interactions.
- Avoiding Chemical Exposure: If you work in an industrial setting, strictly adhere to safety protocols and wear appropriate protective equipment to avoid exposure to hydrogen sulfide and other toxic gases.
For organizations working to raise awareness about various blood health conditions, effective thalassemia affiliates strategies can serve as a model for public health education, emphasizing the importance of genetic testing and safe medical practices.